Study and Validation of a Model
of Fetoplacental Circulation
1.2. Fisiologia della circolazione feto-placentare
Physiology of Fetoplacental Circulation 
|
|
La placenta costituisce l'anello di collegamento tra l'organismo della madre e quello del feto.
Realizza le funzioni di scambio di materia e di termoregolazione.
La corretta perfusione del letto placentare è una prerogativa
indispensabile per una completa crescita e per lo sviluppo del feto; una
conoscenza specifica e il controllo di questa circolazione sono dunque
un fondamentale supporto per l'assistenza delle pazienti gravide.
Ci si potrà rendere conto di un problema che sempre si incontra
affrontando questo tipo di studi: l'estrema varietà e discordanza
di dati disponibili nella letteratura medica in particolare per quanto
riguarda gli aspetti morfologici della placenta e del feto.
1.2. Physiology of Fetoplacental Circulation 
|
|
The placenta is the link between a fetus and its mother
about the exchange of substances and the thermoregulation.
Fig.5: Placental functions. 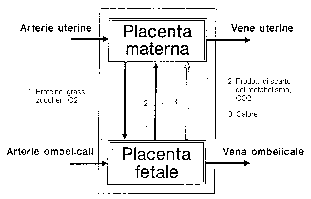
At the childbirth it will be replaced by digestive system, lungs
and kidneys of the newborn, for the exchange of substances.
The thermoregulation will be driven by the central nervous system through
the control of blood circulation and of the metabolism.
Other placental functions:
- Production of hormones
- Transmission of chemical messages
- Regulation of the resistances of the fetal circulation
- Regulation of oxygenation of the fetal blood.
How and how much these functions are achieved is still mainly unknown.
The proper perfusion of the placental vessels is a prerequisite for
the complete growth of the fetus. The specific knowledge and the ability
to control this circulation are the fundamental support for the assistance
to pregnant patients.
This type of research always faces with a problem: the big variety
and and the presence of conflicts among the available data of the medical
literature in particular about the morphology of the placenta. The following
description refers mainly to data from studies developed by well-known
researchers, compared also to the data obtained during our experiments
on several placentas as described in Part 2.
1.2.1. Fetal Circulation . 
|
|
In the fetus, the systemic, pulmonary and umbilical circulations have several links.
The umbilical and placental circulations are a temporary system for the life and the growth of the
fetus, that is abandoned at the childbirth, when drastic changes take place transferring the function
of gas exchange from the placenta to the lungs.
The right and left ventricles, for the existence of two vascular links, the foramen ovalis and the
arterial duct, work in parallel in order to pump oxygenated blood from the placenta through the
umbilical vein [9] to the aorta; about 50% of it (saturated to 80% approximately) does not cross the
liver but the venous duct reaching the inferior cave vein [10], where also blood coming from the
legs flows, lowering therefore the saturation to 70% approximately. Then it flows mainly into the
ascending aorta through the foramen ovalis. The flow of the superior cave vein, rather poor of oxygen,
flows from the right atrium to the right ventricle and subsequently into the descendant aorta through
the arterial duct (Botallo).
The saturation of blood in the descendent aorta and in the following arteries is about 60%.
The blood flow in the first part of the aortic arc is coming from the left atrium. Here, with a modest
amount of blood coming from the lungs (that behave as oxygen consumers in the fetus), also a big part
of the flow of the inferior cave vein (with oxygenated blood from the placenta) arrives. Therefore the
heart and the brain receive a better oxygenation than the organs of the low part of the body.
The aortic blood flows for 60% [11][12] to the placenta and for 40% to the other organs.
Other differences versus the situation of the adult are the relatively high value of cardiac flow, the
high frequency of the heart and the low arterial pressure [9]; the cardiac flow of the fetus is varied
exclusively by the frequency of the pulsations, since the fetus cannot vary the real volume of the
cardiac pulse [13].
From the right ventricle, also the pulmonary circulation is originated, characterized by a high vascular
resistance and a reduced volume of blood.
The pressure in the pulmonary artery is several mmHg higher than in aorta, so a consistent part of blood
flows from the pulmonary artery into the aorta through the arterial duct.
The pressures in the fetal districts are subject to an increment because of the pressure of the amniotic
fluid, which can change according to the maternal intra-abdominal pressure. Therefore we prefer to
consider the values of pressure not relatively to the atmospheric pressure, but to the intra-amniotic
one, as in the figure 7.
Increasing the pressure of the amniotic fluid, an equivalent increase of the pressure of the intervillous
space [14] takes place. The pressure value in the intervillous space is approximately 10-13 mmHg [14],
as confirmed by other authors [15]: in our model this value will be 12 mmHg.
The modifications that happen after the childbirth are evidenced in the schematic diagram in figure 8;
during the birth, the interruption of the placental circulation, the occlusion of the foramen ovalis and
of the arterial duct, and the beginning of the pulmonary activity take place.
After the occlusion of the umbilical vein, the expansion of lungs produces a strong reduction of the
vascular resistance; therefore a marked increase of the pulmonary blood flow [10] can be observed.
The pressure of the left atrium of the fetus reaches values higher than inside the right atrium, causing
the occlusion of the foramen ovalis. Also the arterial duct closes, disappearing within few days.
Fig.6: The fetal circulation.
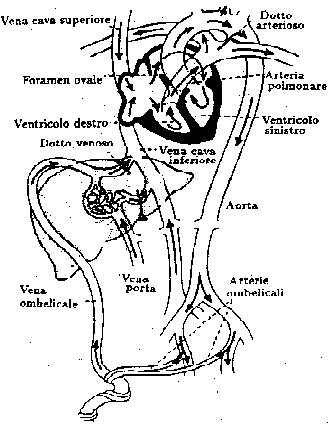
Fig.7: Fetal circulation in the sheep: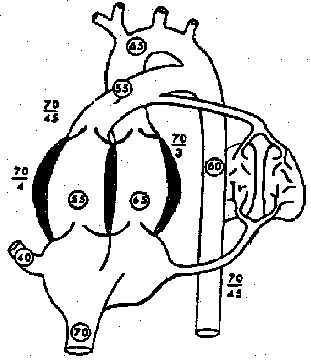
Circled values = of oxygen saturation,
Remaining values = pressures (max/min) relative to the amniotic pressure.
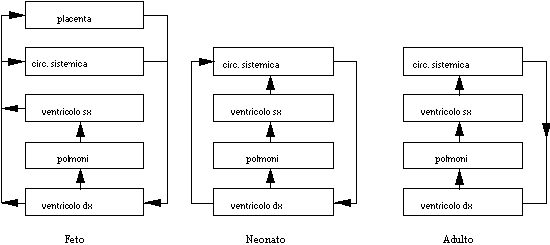
Fig.8: Changes in the circulation from the fetus to the newborn and the adult.
1.2.2. The Placenta: Morphology and Functions . 
|
|
We will describe the placenta from the anatomical point of view, in order to understand its morphology
and its functions, to evaluate the geometric characteristics that will be useful in the development of
our model.
The placenta puts in relation the mother with the fetus supplying feeding and respiratory necessities;
it is a gas exchanger (oxygen and carbon dioxide) between the maternal and fetal blood, that are always
separated; it removes the metabolic products, it controls the temperature of the fetus, it is a filter
against virus and harmful factors; it fulfills also endocrine functions carrying and producing hormones.
At the end of the pregnancy the placenta is an organ of disk shape, 20-25 cm in diameter, 3-4 cm in
thickness, variable weight between 400 and 600 g [16] and 420-490 cm3 [17] in volume. The fetal
circulation is a capillary system in which the relationship surface of membrane / volume is maximized
thanks to cylindrical and spherical geometry; the maternal blood flows around the vascular structures
(villi) while the fetal blood flows into their inner part. The villi are the only parts of the placenta
interested by both the blood flows.
The maternal circulation (intervillous) is a system (maternal pool) where the Fåhreus-Lindqvist effect
can be considered negligible [18]. The villi behave like small obstacles in the blood current [19].
The figure 10 represents the diagrams of blood flows in various types of placental systems, according to
Faber, Moll and Martin [20].
Fig.9: A placenta used for the incannulation tests.
The system of multivillous exchange of the human placenta is not the most efficient: this is confirmed by
the fact that 1 gram of human placenta feeds only 6 grams of fetus, compared to a ratio 1:20 in the
guinea-pig.
Anyway the multivillous system has an advantage: it allows in a better way the continuous adaptation to
conditions that change heavily during the growth.
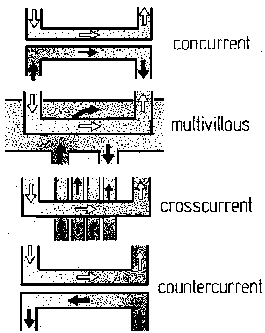
Fig.10:
Types of placental exchange system.
The white arrows indicate the fetal flow, the black ones indicate the maternal flow,
the variation in density of points indicates the efficiency.
1.2.3. Anatomy of the Fetal Side . 
|
|
The fetal surface of the placenta is covered by the amniotic membrane.
The umbilical cord is connected approximately at the center, where, after the chorion, its ramifications
originate the villi, a complex vascular net, that extends similarly to roots in the pool of maternal
blood.
These ramifications, in their final parts, constitute a capillary net in which the fetal blood is
oxygenated. Every main root (main stem villus or stem villus of 1st order) has its own ramifications
that cross the pool until they reach the basal plate of the maternal part; every stem villus with its
ramifications is named cotyledon.
There is a mismatch in the literature on the number of cotyledons, anyway it is not always the same in
every placenta. Wilkin suggests a number between 20 and 40 [21], Novak between 15 and 40 [22], but the
probably most reliable number is approximately 50 ~ 70 at the end of the pregnancy [23][20].
The cotyledons are purely vessels; they are in part berthed to the basal plate and in part free to
fluctuate in the intervillous space. A schematic diagram of the fetal cotyledons is shown in figure
12 [24].
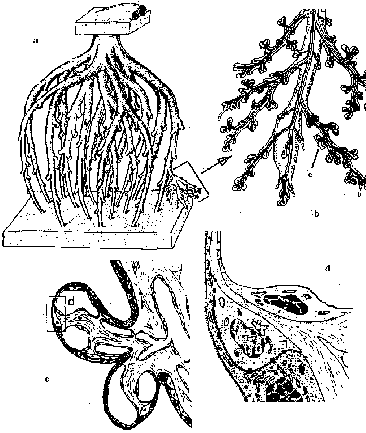
Fig. 12: Morphology of the villi of the human placenta:
a) the cotyledon:
ChP: chorionic plate BP: basal plate
T: trunk I-IV: rami.
b) peripheral ramification of a cotyledon:
1: stem villus 2: mature intermediate villus
3: immature intermediate villus 4: terminal villi.
c) section of two terminal villi.
d) section of the placental barrier.
|
The vascular venous and arterial structures of the villi are almost symmetrical, like in other organs.
The muscular cells of the vessels are relatively dispersed but they have more intercellular connections:
Nikolov and Schiebler (1973) have interpreted this as a muscular system that could be important for an
independent local regulation.
Following the blood flow from the umbilical arteries to the terminal capillaries, we will introduce a
classification of the placental villi, with reference to Kaufmann (1990) [16] and Arts [25].
Kaufmann has obtained his data analyzing sections of tissue obtained from placentas fixed through
immersion in formaline, without perfusion, with the electronic microscope. Arts has analyzed tissues
after the perfusion of the placentas with polimetilmetacrilate and their dissolution through immersion
in KOH.
Following the description of Arts [25] we can classify the placental vessels as follows:
- chorionic vessels;
-
vessels of the cotyledons;
-
capillary vessels in the villi;
-
paravascular capillary network.
The villi can be classified in 5 main groups: stem villi, mature and immature intermediate villi,
terminal villi and to mesenchimal villi [20].
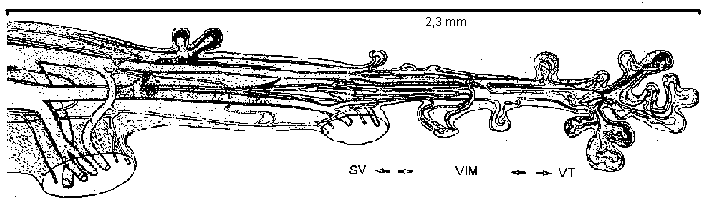
Fig.14: Diagram of a peripheral stem villus.
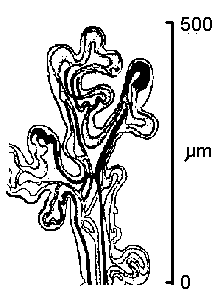 Fig.16: Longitudinal section of a terminal villus.
Fig.16: Longitudinal section of a terminal villus.
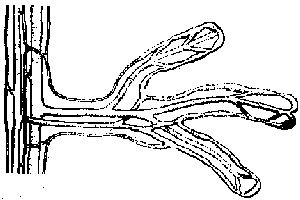 Fig.17: Structure of a villus.
Fig.17: Structure of a villus.
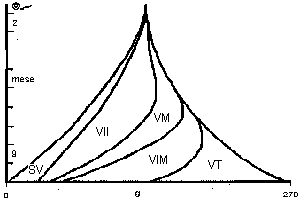
Fig.18: Development of the volume of several the types of villi, versus the gestational age:
SV stem villi 31g 11%
transition to intermediate immature villi 24g 9%
VII intermediate immature villi 9g 3%
VM mesenchimal villi 3g 1%
transition to intermediate mature villi 3g 1%
VIM intermediate mature villi 77g 28%
transition to terminal villi 31g 11%
VT terminal villi 95g 35%
1.2.4. Anatomy of the Maternal Side .
|
|
The external surface of the maternal part is extremely irregular and wrinkled, it is divided in several
lobes; its color is dark red.
The placenta at the end of pregnancy is fed by the uterine arteries that split into 60 ~ 120 spiral
arteries, connected to the basal plate [30]. The utero-placental flow increases during the pregnancy
from 50 cc/min (10 weeks) to 500-600 cc/min. The ratio of uterine blood flow reaching the placenta is
not exactly known; in the late pregnancy, the placenta probably receives 90% of the total flow [30].
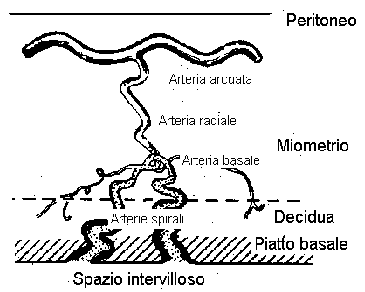
Fig.19: Schematic diagram of the contribution of blood in the intervillous space.
The maternal blood of the spiral arteries flows into a system of communicating interstices that encircles
the cotyledons: the intervillous space. Here oxygen and the nourishing substances of the maternal blood
are exchanged with the fetal blood and at the same time the products of the fetal metabolism are acquired.
Then the maternal blood flows into the veins of the basal plate ("physiological" model of Ramsey) [31].
Each villous tree depends on its spiral artery: although the intervillous space is a system rather open,
the disposition of the villi and the gradient of pressure are linked so that the perfusion depends
closely on the original placement of the flows [32]: the occlusion of a spiral artery causes the death
of the tissue of the cotyledon that it used to feed.
The blood pressure at the end of the spiral arteries is approximately 70 mmHg, in the intervillous space
it is 12-15 mmHg [15] and in the endometrial veins, where blood is drained, it is 8 mmHg: the
pressure gap is almost totally in the intervillous space.
The studies of Freese explained that the cotyledons do not grow in uniform way but leave cavities in
front of the orifices of the spiral arteries. The maternal blood from the basal plate enters in this
empty space and, pushed by the pressure, flows towards the chorion (fig. 14), it passes through the
cotyledons not dispersing itself and finally it is drained by the endometrial veins.
best viewed with  res. 800 x 600.
res. 800 x 600.
Last updated: July 5, 2008: banner exchange removed.






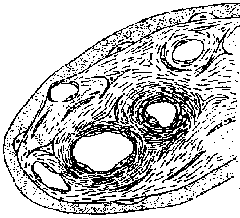 Fig.13: Cross-section of a stem villus.
Fig.13: Cross-section of a stem villus.
 Fig.16: Longitudinal section of a terminal villus.
Fig.16: Longitudinal section of a terminal villus. Fig.17: Structure of a villus.
Fig.17: Structure of a villus.
