Nursing Process: ASSESSMENT

The nurse collects data about the health status of the client. The data is
subjective and objective.
Subjective data is usually documented in the clients own words. This data includes such things as previous experiences, and sensations or emotions that only the client can describe.
The Objective data is obtained by the health team, through observation, physical examination, or/and diagnostic testing. Objective data can be seen or measured.
Sources of
subjective data and objective data are the client, the family and significant
others, medical records, and other health care team members.
Assessment includes, the "HEALTH
HISTORY" and "physical assessment".
Physical assessment can be broken down into four components;
- Inspection,
- Palpation,
- Percussion,
- Auscultation.
CLICK on the
above links to obtain further information.
Measurement Criteria(2)
- The priority of data collection is determined by
the client's immediate condition or need.
- Pertinent data is collected using appropriate
assessment techniques.
- Data collection involves the client, significant
others, and health care providers when appropriate.
- The data collection is ongoing.
- Relevant data is recorded according to
standards.
NOTE: For the purpose of examples of Nursing Process, I will be using the
following Case Study through out this report.
Client with Liver Disease - Cirrhosis
Disease Backgrounder:
Cirrhosis is a condition that results from permanent damage or scarring of the liver. Diffuse disorganization of normal hepatic structure by regenerative nodules that are surrounded by fibrotic tissue. This leads to a blockage of blood flow through the liver and prevents normal metabolic and regulatory processes.
As liver function decreases, fewer proteins such as albumin are produced resulting in fluid accumulation in the legs (edema) or abdomen (ascites). Individuals with cirrhosis may bleed and bruise easily due to a decrease in proteins required for blood clotting. Some people may even experience intense itching due to products that are deposited in the skin.
In the Western world, cirrhosis is the third leading cause of death in patients aged 45 to 65 (after cardiovascular disease and cancer); most cases are secondary to chronic alcohol abuse.
Nursing Process: HEALTH HISTORY

The health history is a collection of subjective data that includes
information on both the client's past and present health status. It is used in
conjunction with the physical examination and laboratory findings as a basis
for drawing conclusions about an individual's state of health. It allows
positive aspects, health problems, health habits as well as abnormal symptoms,
health problems, health teaching needs, and health concerns to be identified.(2)
Components of a comprehensive Health History
- Date history obtained.
- Source of history.
- Interpreter if used.
- Reason for seeking health care.
- Client Profile Data.
- Present Illness Data.
- Present Health Status.
- Past Personal data.
- Family Medical data.
- Life-style data.
- Health Management data.
- Psychological data.
- Review of Systems.
Guidelines for Obtaining a Health History(2)
- Greet client by name.
- Introduce yourself and your designation, what
you are intending to do.
- Provide a private , quiet environment, free of
interruptions.
- Ensure client is comfortable.
- Ask one question at a time.
- Ask direct questions.
- Avoid leading questions.
- Do not "put words in the clients
mouth"; Allow the client to use his or her own words.
- Give the client your undivided attention and
acknowledge listening by nodding and saying " uh hum".
- Promote accurate, complete communications.
- Be alert to non-verbal communications.
- Take brief notes.
NOTE: For the purpose of examples of Nursing Process, I will be using the
following Case Study through out this report.
Client with Liver Disease - Cirrhosis
Health History:
Mr. K is a 45 year old polish male. Married with three children. He
is currently unemployed. He has worked in the service industry for his entire
life. He has been socially drinking since he was 13 yrs. He has a family
history of alcoholism and diabetes.
Past Medical History:
- Previous liver disease, hepatitis B
immunization, no medications except cold remedies. Father died of cancer,
mother alive. Usual childhood illness, broken leg at age 16, no surgeries.
He has been admitted to ICU on three previous occasions for liver disease.
Presenting Complaint:
- Fatigue, weight changes, digestive disturbances,
skin changes, weakness, pruritis, dyspnea, anorexia, abdominal pain,
nausea, and vomiting, diarrhea, bloody stools, changes in urine or color,
numbness or tingling of extremities
Physical Examination:
Vital Signs: B.P. 160/90(hypertension), respirations:28(tachypnea), pulse:96
Height and Weight:5ft., 10in.,77kgs.
Skin: Dryness, scratches, jaundice, bruises
Eyes: Scleral icterus
Thorax: Spider angiomas
Breast: Gynecomastia
Abdomen: Distention, prominent veins, girth:715cm., liver enlargement
Nursing Process: PHYSICAL ASSESSMENT:INSPECTION
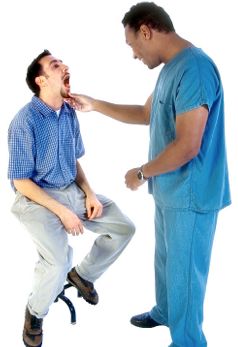
INSPECTION Defined:
Inspection is the visual examination of the client.
Guidelines for Effective Inspection
- Be systematic
- Fully expose the area to be inspected; cover
other body parts to respect the client's modesty.
- Use good light, preferably natural light.
- Maintain comfortable room temperature.
- Observe color, shape, size, symmetry, position,
and movement
- Compare bilateral structures for similarities
and differences.
Nursing Process: PHYSICAL ASSESSMENT:PALPATION
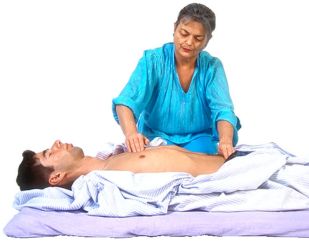
PALPATION Defined:
Palpation uses the sense of touch to assess various parts of the body and helps to confirm findings that are noted on inspection.
The hands, especially the finger tips are used to assess skin temperature, check pulses, texture, moisture, masses, tenderness , or pain.
Ask the Client for permission first and explain to your client what you intend to examine. Establish client trust with being professional. Please remember to use warm hands.
Any tender areas should be palpated last.
Types of Palpation:
- Light Palpation: To check muscle tone and assess
for tenderness
- Deep Palpation: To identify abdominal organs and
abdominal masses.
Note when examining Abdomen, you auscultate first followed by percussion
then palpation.
Nursing Process: PHYSICAL ASSESSMENT:PERCUSSION
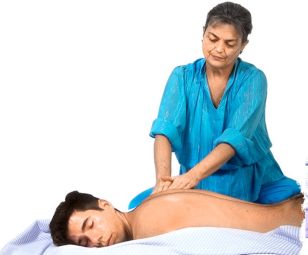
PERCUSSION Defined:
Percussion is the striking of the body surface with short, sharp strokes in order to produce palpable vibrations and characteristic sounds. It is used to determine the location, size, shape, and density of underlying structures; to detect the presences of air or fluid in a body space; and to elicit tenderness. (2)
Note when examining Abdomen, you auscultate first followed by percussion then palpation.
Types of Percussion
- Direct Percussion: Percussion in which one hand
is used and the striking finger of the examiner touches the surface being
percussed.
- Indirect Percussion: Percussion in which two
hands are used and the plexor strikes the finger of the examiner's other
hand, which is in contact with the body surface being percussed.
- Blunt Percussion: Percussion which the ulnar
surface of the hand or fist is used in place of the fingers to strike the
body surface, either directly or indirectly.
Percussion Sounds
- Resonance: A hollow sound.
- Hyperresonance: A booming sound.
- Tympani: A musical sound or drum sound like that
produced by the stomach.
- Dullness: Thud sound produced by dense
structures such as the liver, and enlarged spleen, or a full bladder.
- Flatness: An extremely dull sound like that
produced by very dense structures such as muscle or bone.
Nursing Process: PHYSICAL ASSESSMENT:AUSCULTATION

AUSCULTATION defined:
Auscultation is listening to sounds produced inside the body. These include breath sounds, heart sounds, vascular sounds, and bowel sounds. It is used to detect the presence of normal and abnormal sounds and to assess them in terms of loudness, pitch, quality , frequency and duration.
Note when examining Abdomen, you auscultate first followed by percussion then palpation.
Nursing Process: Definition |
Critical Thinking
| Guidelines
Critical Thinking:
Characteristics
| Skills, Elements, Standards
Nursing Process: Assessment
| Nursing
Diagnosis | Planning | Implementation | Evaluation
John
Philip Tiongco, MD