Israeli Paramedics Association
Transcutaneous Pacemaker
By
Paramedic Neomi Zvi
Israel. The night between Thursday and Friday.
The evening MICU�s team was back to the station long after their shift was
over. The MICU was �half empty�. �Go Home� I said to the �evening
paramedic� , I�ll complete the missing equipment and fill the 3 empty �D�
Oxygen cillinders.
7 minutes later we (Dudi the EMT-B and me) were dispatched to:
�A 54 y/o lady with shortness of breath�
0n the scene 00:55
The lady , about 140 kg (309 pound) , with no legs from the knee down
(Emputations of both lower extremities due to severe Diabetes) .
According the pt�s daughter � she is �not feeling well� since late after noon
and dramatically deteriorating in the last 10 minutes. Medications: Insulin.
The pt looked as in shock. Pail , sweating , semiconscious , spontaneously
breathing , about 25 / min , little snoring , (A slight extension of the pt�s
head , her airway was adequately open and she stopped snoring) . No
evidence for ulmonary Edema.
No Radial pulse , Carotid Pulse- less then 30 / min , regular �
�You don�t want Intubation?�
asked the EMT-B and connected the pt to the Oxygen mask I ordered.
�No , not now anyway� I answered.
While Dudi attached the monitor cables , I open an IV line (and drew blood
for sugar level � it was 450 mg%) and put the 500cc Ringer�s Lactate to �run�.
On the monitor - C.AVB (3rd degree AV Block) .Systolic BP - 60 mmHg.
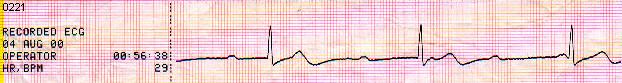
Dudi was watching the pt�s Airway / Breathing � like a Falcon after his prey ��.
Midazolam 2.5 mg IV --> External Pacemaker , aimed to rate of 100 / min
(as a start) and I got the desired �capture� only at current of 120 MA at first
and then down to 80 MA and the same I did with the pacemaker rhythm.
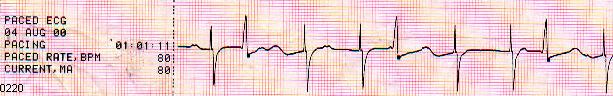
A thready Radial pulse of 100. Systolic BP � 75 mmHg .
Dudi called for the BLS backup and asked them to bring upstairs the
backboard and safty belts (There is no other way we could get her
downstairs )
In the mean time , second IV line , Ringer's + parallel of Sodium Chloride
0.9% with Dopamine and only then we got a Systolic BP of 90 mmHg.
Now the Pulse Oximeter could detect her SaO2 ...96-97%...
It took to all 4 of us almost 10 minutes to get her down through the
narrow stair's room , (No balance , heavy weight and the short Pacemaker
cables of the LP 10 did not help either�)
No need to tell you how HARD it was -
Each floor we stopped for few seconds to detect the pt vital signs and the
pacemaker attachments�.. She was doing relatively ok.
We just loaded the pt into the MICU , and all of a sudden her
breaths became irregular and in front of my eyes the rhythm on the
monitor has change into
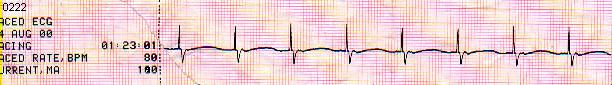
I immediately rechecked the pt as well as the pacemaker��
Well , the pacemaker was ok � but the lady was not.
Her consciousness was deteriorating , still have few "breaths"......no
Carotid pulse.
I removed the Oxygen mask out of her face , Tilting the head back (short
neck...) Oropharyngeal AW , Ventilation with BVM, O2 , Chest
Compressions , quick Intubation
I turned the pacing off for few seconds to confirm the base rhythm of the
pt � I suspected she went into��.and put it on again
Asystole on the monitor (Witnessed Asystole..)

After about 50 seconds , the pulse and breathing were back and few
seconds later the pt was half awake again . On the monitor � CAVB ,
demand pacemaker �
I had to sedate her again � due to pacing and the ETT.
The Dopamin drip was still needed
I�v asked the BLS team to spilt � and Hannan , the EMT-B helped me
on the way , while his partner is following our MICU with his ambulance.
Dudi was driving to the hospital when the pt went into Asystole again
CPR for less then a minute � and she is back again � with spontaneous
Pulse and Breathing , CAVB , Pacemaker with good cupture and BP of
100 / 65 mmHg..
This episode of Cardiac Arrest repeted it self 3 times till we arrived to the
Hospital.
The funny thing was that sometimes her brain did not have enough time
to react (lose consciousness) to the Cardiac Arrest�(we were quicker)
In the Hospital:
We brought her to straight into the ICCU with SaPO2 of 99% ,
Half awake - trying to extubate herself (got another dose of Midazolam),
External Pacemaker at rate of 80/min at current of 80 MA , Palpated
pulse of 110 / min (Pacemaker beats + pt's spontaneouse pulse) , BP
of 135/90 mmHg , Nerrow and good reactive pupils.
Code Summary strip x 2 (one for the ICCU records and one for my
students) . Apologizing to the ICCU docs for not having the time to
performed 12 leads ECG , and explanations why the pt is on a
back board.
Outcome:
After one week , or so � she was back home with her brand new permanent
Pacemaker and with much more balanced Electrolytes.
Paramedic Neomi Zvi - Jan 2000