Alimentary tract and pancreas
Alimentarni trakt i pankreas
ARCH
GASTROENTEROHEPATOL 2002; 21 ( No 1 – 2 ):
Stenosis of
the small intestine and entero-enteral fistula due to mesenteric vascular
occlusion
Stenoza tankog creva i entero-enteralna fistula prouzrokovani
mezentericnom vaskularnom okluzijom
( accepted April 24th, 2002 )
Zoran Krivokapic, Radoje Colovic, Nikica Grubor, Marjan Micev
Institute for Digestive Diseases, Clinical Centre of Serbia, Belgrade.
Address corresponence to: Professor Dr Zoran Krivokapić
Instut za digestivne bolesti, KCS
6 Koste Todorovića Str,
YU-11000 Beograd, Serbia, Yugoslavia.
Tel./Fax: +381 11 361 8669
E-mail: [email protected]
……………………….
………………………………….
Entero-enteral fistula due to mesenteric occulsion Gastroenterloska sekcija SLD-
01728, 2002.
ABSTRACT
Stenosis of the small bowel due to mesenteric ischemia is rare and, to our best knowledge, a case of the entero-enteral fistula caused by that condition has not been described in literature so far. According to the clinical picture, patological features and localization, small bowel ischemic strictures can be divided into two groups: First, where ischemia goes unnoticed with symptoms only when intestinal stenosis is developed and where a short segment of the bowel is affected, and second, with episodes of acute ischemia followed by asymptomatic periods as well as by symptoms of intestinal obstruction, where the involved segment is longer and usually localized in jejunum. The diagnosis is based on the history, enteroclysis and pathohystological examination. In the differential diagnosis Crohn's disease and others causes of the acquired stenosis of the small bowel have to be considered. The therapy is surgical implying the removal of the stenosed segment of the small bowel with the additional angioplastical operation, when necessary.
We present a case of 66-year old patient previously treated for mesenteric vascular occlusion with instillation of Novocain solution in the radix of the mesentery. The diagnosis of intestinal stenosis was established by upper GI series and confirmed itraoperatively. Double jejunal stenosis was found. Segmental resection of the affected intestine and end-to-end anastomosis were performed. Examination of the resected specimen revealed a jejuno-jejunal fistula in the stenotic segments. Crohn's disease was ruled out. The postoperative course was uneventful and the patient was discharged several days later. He is symptom-free three months after surgery.
Key words: mesenteric
ischemia, intestinal obstruction, entero-enteral fistula.
SAZETAK
Stenoze tankog creva prouzrokovane mezenterijskom sudovnom ishemijom su retke. Prema nasem uvidu u medicinsku literaturu slucaj entero-enteralne fistule prouzrokovane ovakvim stanjem do sada nije opisan. Zavisno od klinicke slike, patoloskih promena i lokalizacije, ishemijske strikture tankog creva mogu da se podele u dve grupe. U prvu grupu spadaju ishemije koje prolaze klinicki nezapazeno i koje se ispoljavaju tek onda kada nastanu simptomi stenoze tankog creva. U drugoj grupi su slucajevi u kojih su epizode crevne ishemije manifestne i iza kojih sledi asimptomski period sve do ispoljavanja simptoma i znakova stenoze tankog creva. Dijagnoza se zasniva na anamneznim podacima, enteroklizi, i patohistoloskom pregledu reseciranog dela creva. U diferencijalnoj dijagnozi uvek treba da se razmotri Crohn-ova bolest i drugi uzroci stecenih stenoza tankog creva. Lecenje je hirursko i podrazumeva odstranjenje stenozantnog segmenta sa dodatnom angioplastikom ukoliko je to indicirano.
U radu se prikazuje slucaj pacijenta zivotne dobi 66 godina koji je prethodno bio lecen od mezenterijske vaskularne okluzije instilacijom Novocaina u radiks mezenterijuma. Dijagnoza intestinalne stenoze je postavljena radioloskim pregledom alimentarnog trakta. Itraoperativno je otkrivena dvostruka stenoza jejunuma. Segmentna resekcija izmenjenog dela creva i termino-terminalna anastomoza je bila nacinjena. Pregled reseciranih delova creva je otkrio jejuno-jejunalnu fistulu u stenoticnom segmentu. Crohno-va bolest je bila iskljucena. Postoperativni tok je bio bez komplikacija i pacijent je otpusten desetog dana izlecen.
Kljucne reci: mesentrijska ishemija, intstinalna opstrukcija, entero-enteralna fistula.
Ischemic disease of the small intestine is not frequent. In the acute form it is characterized with high mortality (over 50%). To our best knowledge, small bowel stenosis due to mesenterial ischemia is rare, while entero-enteral fistula caused by ischemia has not been described until now.
Case report
Four
months before admission to our institution, the patient, a 66 years old
man, undergone emergency explorative
laparatomy due to simptoms and signs of mesenteric ischemia. The patient has
passed medical history of arterial
hypertension for about 30 years. He experienced acute myocardial infarction in
1979, and in 1983 a triple arteriocoronary bypass due to coronary disease. He
never used digitalis or potassium chloride medication. At operation mesentery
radix was infiltrated with Novocain solution resulting in improvement of bowel
perfusion thus making the bowel resection unnecessary. Three months later he
became pyrexial. Nausea and protracted diarrhoea appeared as well.
During the following month, most of the
symptoms abated except abdominal colic, malaise, and progressive weight loss.
Physical examination revealed no abnormalities except mild tenderness of the
lower abdomen. Laboratory findings were within the normal limits. Plain
abdominal x-ray films demonstrated air-fluid levels. Barium enema and
sygmoidoscopy were suggestive of dolichocolon. Examination of the small
intestine with enteroclysis showed presence of two jejunal stenosis with large
prestenotic dilatations. Figure 1. Doppler ultrasonography of
portal system did not reveal any pathological findings. There were no signs of
thrombosis, decreased flow or presence of collateral venous vessels. Abdominal
aortography and selective visceral angiography showed: stenosis of the coeliac
trunc up to 60-70%, occlusion of superior mesenteric artery in the middle part
with rich collateral vascularisation and an arcus of Riolan that vascularised
the coecum with normal features of mesenteric and portal veins. Figure 2. Accordingly, mesenteric
ischemia was recognized as the aetiological factor. The patient was operated on
26.07.1999. After the adhesions were removed a subtotal occlusion of the small
intestine, 80-100 cm of Treitz and an
intestinal jejuno-jejunal fistula was found. Figures
3,4. Resection of the affected segment of the small intestine was
performed in the length of 70 cm with a stapled side-to-side anastomosis.
Postoperative recovery was uneventful. The patient was discharged 9 days after
the operation and was symptom-free at the time. On the last follow-up
examination the patient had no complaints. Histopathological examination of the
resected part of the small intestine showed chronic inflammation of the mucosa
with ulceration, Crohn’s disease-like chronic lymphocytic inflammation of the
submucosa without granulomata or other
histopathological features of Crohn’s disease. This was nonspecific
finding that might correspond to the ischemic origin of the changes.
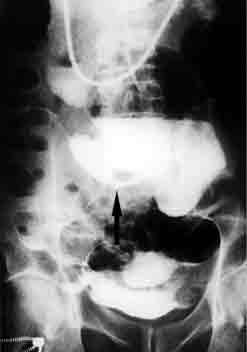
Figure 1.
Enteroclysis showing two jejunal stenosis
with prestenotic dilatations

Figure 2. Abdominal aortography and
selective visceral angiography showing stenosis of the celiac truncus,
occlusion of superior mesenteric artery with rich collateral vascularisation.
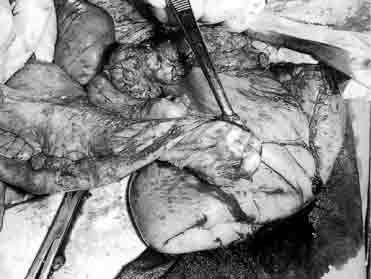
Figure 3.
Stenosed jejunal segment with large prestenotic dilatation
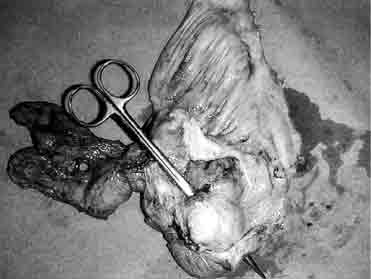
Figure 4. Resected
specimen showing stenosis of the small bowel with prestenotic dilatation and
jejuno-jejunal communication (fistula).
Discussion
Mesenteric ischemia can be chronic, with functional bowel changes (malabsorption), but without
impaired intestinal vitality or acute,
where ischemic damage of the bowel is so severe that jeopardizes the vitality
of the intestine thus leading to structural changes. In the acute mesenteric
ischemia, ischemic damage may vary from transient impairment of the bowel
function to transmural ischemic necrosis resulting in intestinal perforation.
Between these two extremes is the so-called “subnecrotizing ischemia”, when ischemic lesion does not damage all
layers, but the mucosa only, which is the most vulnerable to ischemia (1).
Resistance to ischemic damage rises from the lumen inside out. The level of
ischemic damage progression depends on the degree of ischemia and of efficacy
of compensatory mechanisms. When ischemic damage reaches the lamina muscularis
mucosis, then it leads to formation of fibrous tissue and, subsequently, to
retraction and formation of the bowel stenosis (2). Acute mesenteric ischemia
usually is so severe that in more than 50% cases of cases it ends lethally (3).
All causes of acute mesenteric ischemia belong to this type of ischemic damage.
Thrombosis of the superior mesenteric vein is very rare (4). Embolisation of
the superior mesenteric artery (SMA), thrombosis of the SMA, nonocclusive
ischemic disease and, especially, focal segmental ischemia are causes of
ischemic intestinal strictures ( 5,6,7). In embolisation of the SMA major
emboli may be present in 85-90%, usually lodged in the beginning of ileocolic
artery and minor emboli, present in 10-15%, in the distal part. The latter are
mostly the cause of intestinal stenosis (2). Experimental studies support that
opinion. Embolisation of branches of the SMA in dogs with gelatin sponges
provoked segmental intestinal stenosis (8). Reasons for focal segmental
ischemia of bowel include atheroembolism, strangulated hernias, vasculitis,
blunt abdominal trauma, segmental venous thrombosis, radiotherapy, drugs (oral
contraceptives, digoxins, NSAID, cocaine) where, due to a range of damage of
the intestinal vascular bed, adequate collateral circulation prevents
transmural necrosis of small intestine (2,9.10). That is the reason why acute
focal segmental ischemia is probably the
most common cause of the ischemic bowel stenosis. Clinical manifestations of
mesenteric ischemia correlate with the level of ischemic damage of the bowel,
and less with the underlying cause (2).
Based on histopathological findings, clinical picture and evolution of the disease, we can divide all acquired ischemic strictures of the small bowel into two major types (11):
1) Asymptomatic form of mesenteric ischemia. This
clinically manifests with insidously but progressively developing intestinal
obstruction. Usually short segment of the small intestine is affected (usually
middle or terminal ileum). .
2) Symptomatic form is when symptoms and signs of
the acute mesenterial ischemia are
present from the beginning. This was followed by asymptomatic period and
gradually developing symptoms and signs of the intestinal occlusion thereafter.
In this case larger part of the bowel, oftenly jejunum, is affected.
It is not always possible to make a clear distinction between these two types of intestinal ischemic strictures, since transitive forms and variations are not rare (5,7,12,13). Our patient, however, fits into to this classification. Kradijan and associates described 6 patients with large ischemic lesions of the small intestine who had an asymptomatic phase followed by clinical picture of ileus and perforation in two cases. The strictures were localized in the ileum and involved short segments up to 3 cm in length, with normal appearance of bowel under stenosis. The confusion is produced by the fact that 5 of 6 patients had enteric-coated potassium chloride in therapy, later found to be the culprit of formation of strictures and bowel perforation, while the lesions completely matched the lesions accompanying this form of medication, in their appearance (pylorus-like annular and tubular stenoses) and localization (distal ileum) (14).
It difficult to determine why ischemic
stricturing is more frequent in certain portions of the small intestine. This
is partly due to poor vascularisation of
the terminal part of the ileum and rich vascularization of the jejunum.
That is the reason why larger segment of the jejunum can be involved with
ischemic process without causing a perforation, but only stenosis. Macroscopic
and radiographic appearance of this
type, where stenosis involves long segments of the small bowel, is similar to
findings in the Crohn’s disease. Therefore, histopathological examination is
necessary for differential diagnosis (1,5,11).
It is important to distinguish ischemic
strictures from nonischemic ones due to Crohn’s disease, neoplasm, other
inflammatory tumors (for example, acute pancreatitis), use of enteric-coated
potassium chloride, and cause of
intestinal ischemia: trauma, irradiation, mechanical occlusion,
vasculitis, drugs (NSAID’s, digitalis, oral contraceptives), embolisation or
thrombosis of the mesenteric artery, because further treatment depends on this
(7,15).
The diagnosis of the intestinal stenosis is
simple. Contrast radiography of the small bowel is the diagnostic modality of
choice in such a case (16). Ischemic small intestinal lesions may often be the
cause of the acquired small bowel stenosis and therefore angiographic
examinations are necessary to diagnosed it.
The treatment includes resection of strictured
segment of the small intestine and end-to-end anastomosis. Also, depending on
the cause of ischemia, reconstructive surgery of mesenteric arteries directed
towards improvement of perfusion of mesenteric
vascular bed is required, as well discontinuation of related drugs. Therefore,
depending of the cause of intestinal stenosis the type of treatment is not
limited only to resection of stenotic segment.
In conclusion, our case of double jejunal stenosis and jejuno-jejunal
fistula was caused by mesenteric ischemia, namely SMA
thrombosis, which was of limited range due to the localization and previous
intraoperative Novocain treatmen. According to these facts and to angiography
findings, which showed well developed collateral circulation, the treatment was
limited to resection of the stenotic segments. The continuity of digestive
tract was established with
termino-terminal jejuno-jejunal anastomosis.
References:
1. Wayt DM, Helwig EB: Small-bowel ulceration- iatrogenic or multifactorial origin? Amer J Clin Path 1968,49:26-40.
2. Brandt LJ, Smithline AE: Ischemic lesions of the bowel. In Feldman M, Sleisenger MH, Scharschmidt BF (eds): Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology, Diagnosis, Management, ed 6. Philadelphia, WB Saunders, 1998, pp 2009-2024.
3. Bastidas JA, Reilly PM, Bulkley GB: Mesenteric vascular insufficiency. In Yamada Y, Alpers DH, Owyang C et al (eds): Texbook of Gastroenterology, ed 2. Philadelphia, JB Lippincott, 1995, pp 2490-2523.
4. Eugene C, Valla D, Wesenfelder L et al. Small intestine stricture complicating superior mesenteric vein thrombosis. A study of three cases. Gut 1995; 37: 292-5.
5. Feurle GE, Haag B. Acute small bowel ischemia without transmural infarction. Z Gastroenterol 1991; 29: 349-52.
6. Thaker P, Weingarten L, Friedman IH. Stenosis of the small intestine due to nonocclusive ischemic disease. Arch Surg 1977; 112: 1216-7.
7. Saegesser F, Borgeaud J, Schnyder P et al. Stenosis of the small intestine of ischemic origin in the adult. Schweiz Med Wochenschr 1976; 106: 367-76.
8. Cho KJ, Schmidt RW, Lenz J. Effects of experimental embolization of superior mesenteric artery branch on the intestine. Invest Radiol 1979; 14: 207-12.
9. Allen JC. Post-traumatic small bowel obstruction. J R Army Med Corps 1994; 140: 47-8.
10. De Backer AI, De Schepper AM, Vaneerdeweg W, Pelckmans P. Intestinal stenosis from mesenteric injury after blunt abdominal trauma. Eur Radiol 1999; 9: 1429-31.
11. Mozes M, Adar R, Tsur N et al. Intestinal obstruction due to mesenteric vascular occlusion. Surg Gynecol Obstet 1971; 133: 583-7.
12. Haraguchi M, Matsushima S, Fujie Y, Sugimachi K: Ischemic stricture of the jejunum-report of a case. Jpn J Surg 1990,20:715-719.
13. Kradjian RM. Ischemic stenosis of small intestine. Arch Surg 1965; 91: 829-34.
14. Grosdidier J, Boissel P, Bresler L, Vidrequin A. Stenosing and perforated ulcers of the small intestine related to potassium chloride in enteric-coated tablets. Apropos of 11 cases. Chirurgie 1989; 115: 163-9.
15. Kato T, Morita T, Fujita M et al. Ischemic stricture of the small intestine associated with acute pancreatitis. Int J Pancreatol 1998; 24: 237-42.
16. Ginai AZ, Hussain SM, Hordijk ML, den Hollander JC. Case report: solitary ischaemic small bowel stenosis. Br J Radiol 1994; 67: 405-7.
17. Lietz H, Meissner K. Mysterious segmental stenosis of the small intestine. Dtsch Med Wochenschr 1982; 107: 299-303.
Figure 1. Enteroclysis showing two jejunal stenosis with prestenotic dilatations.
Figure 2. Abdominal aortography and selective visceral angiography showing stenosis of the celiac truncus, occlusion of superior mesenteric artery with rich collateral vascularisation.
Figure 3. Stenosed jejunal segment with large prestenotic dilatation.
Figure 5. Resected specimen showing stenosis of the small bowel
with prestenotic dilatation and jejuno-jejunal communication (fistula).