
Trigeminal Neuralgia
Overview
Trigeminal neuralgia, also known as tic douloureux, is an
inflammation of the trigeminal nerve causing extreme pain and muscle
spasms in the face. It usually occurs in adults and may affect those with
multiple sclerosis. Although the exact cause of trigeminal neuralgia is
not understood, several treatments can effectively relieve pain. Each
treatment offers benefits, but each has limitations. You and your doctor
should determine which treatment is best for you.
|
What Is Trigeminal Neuralgia?
Neuralgia is severe pain caused by injury or damage to
a nerve. Trigeminal neuralgia is a painful disorder of the fifth
cranial nerve, called the trigeminal nerve. This nerve arises in the
brain, supplying feeling and movement in the face (Fig 1).
Also called tic douloureux because of the
uncontrollable facial twitching caused by the pain, trigeminal
neuralgia is serious because it interferes with many aspects of a
person's life. "Typical" trigeminal neuralgia involves brief
instances of intense pain, like an electrical shock in one side of
the face. This pain comes in repeated waves that last an hour or
more. A less common form of the disorder, called "atypical"
trigeminal neuralgia, causes a less intense, constant, dull burning
or aching pain. This pain sometimes occurs with occasional electric
shock-like stabs that may last a day or more. |
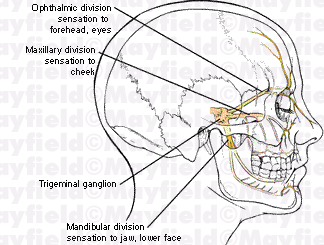
Figure 1. The trigeminal nerve has
three divisions that branch from the trigeminal ganglion: the
ophthalmic division, maxillary division, and the mandibular
division. |
What Triggers A Painful Attack?
When the trigeminal nerve becomes irritated, an attack of
intense pain results. Patients describe an attack as a "pins and needles"
sensation that turns into a burning or jabbing pain, or as an electrical
shock that may last a few seconds or minutes. In some cases of extreme
pain, patients have even considered suicide. Everyday activities can
trigger an episode. Some patients are sensitive in certain areas of the
face, called trigger zones, which when touched cause an attack (Fig. 2).
These zones are usually near the nose, lips, eyes, or ear.
|
Therefore, some patients avoid talking, eating, kissing, or
drinking. Other simple activities, such as shaving or brushing
teeth, can also trigger pain. The pain of trigeminal neuralgia
usually has the following features:
- Typically affects one side of the face
- Can last several days or weeks, followed by a remission for
months or years
- Frequency of painful attacks increases over time and may
become disabling
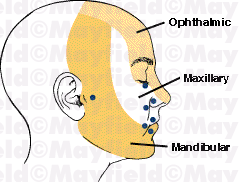
Figure 2. Facial areas of trigger zones.
Trigger points (circles) have the greatest
sensitivity. |
 |
What Causes Trigeminal Neuralgia?
Many believe that the protective sheath of the trigeminal
nerve deteriorates, sending abnormal messages along the nerve. Like static
in a telephone line, these abnormalities disrupt the normal signal of the
nerve and cause pain. Several factors can cause the deterioration of this
protective sheath: aging, multiple sclerosis, tumors, but most doctors
agree that it is caused by an abnormal vein or artery that compresses the
nerve.
Some types of facial pain can result from an infected tooth,
sinus infections, or previous nerve injury. Because the causes of pain
vary, each patient should undergo a medical evaluation.
Who Is Affected?
Trigeminal neuralgia affects 1 in every 25,000 people, and
occurs slightly more in women than men. Patients are usually middle age
and older. Some people with multiple sclerosis also develop trigeminal
neuralgia.
Where To Get Help?
When a person first experiences facial pain, the primary
care doctor or dentist is often consulted. If the pain requires further
evaluation, a consultation with a neurologist or a neurosurgeon may be
recommended.
How Is a Diagnosis Made?
Few causes of trigeminal neuralgia are serious. However, the
possibility of a tumor or multiple sclerosis must be ruled out. Therefore,
the doctor or neurologist will prescribe an imaging study, such as a
computed tomography (CT) or magnetic resonance imaging (MRI) scan. The
diagnosis of trigeminal neuralgia is made after carefully assessing the
patient's symptoms.
What Treatments Are Available?
A variety of treatments are available, including
medications, surgical treatments, and radiosurgery. The first treatment
option is usually medical.
Medications
- Analgesics such as aspirin
and ibuprofen are generally not effective against trigeminal neuralgia.
- Anticonvulsants, such as carbamazepine (Tegretol),
phenytoin (Dilantin), gabapentin (Neurontin), lamotrigine
(Lamictal), and oxcarbazepine (Trileptal), are commonly used because
they block firing of the nerve. These medications are initially
effective for pain control in 90% of patients. These drugs can cause
side effects (e.g., drowsiness, unsteadiness, nausea, skin rash, blood
disorders). Therefore, patients are monitored routinely and undergo
blood tests to ensure that the drug levels remain safe and that the
patient doesn't develop blood disorders. Medications are used as long as
the pain is controlled and the side effects do not interfere with a
patient's activities. When medication is no longer effective, surgical
procedures may be considered. Approximately 25% of patients achieve
long-term relief with medications.
- Muscle relaxants such as baclofen (Lioresal) are
sometimes effective in treating trigeminal neuralgia. Sometimes multiple
drug therapy is necessary to control pain (e.g., Tegretol and
Neurontin).
Surgical procedures
Medications sometimes fail to control pain or cause side
effects. When this happens, the neurologist may suggest that the patient
consult a neurosurgeon, who may recommend one of several surgical
procedures. No one surgical procedure is best for everyone and each
procedure varies in its effectiveness versus side effects (see Comparison of Treatment
Results for Facial Pain). Among the current treatment options,
microvascular decompression (MVD) and percutaneous stereotactic
radiofrequency rhizotomy (PSR) have comparable rates of pain relief that
are highest among the available options. In a review of series of
approximately 100 patients or more published in the past
10 years, the rates of pain relief calculated were 77% in 7 years for MVD
and 75% in 6 years for PSR rhizotomy.
- Percutaneous
stereotactic radiofrequency rhizotomy (PSR), also known as electrocoagulation, produces
a heating current to destroy some of the trigeminal nerve fibers that
produce pain. PSR eliminates pain but also causes partial numbness of
the face. This outpatient procedure is performed under local anesthesia
and sedation. While the patient is awake, an electrode is passed through
the cheek to stimulate the nerve and locate the pain-causing area. The
patient is then anesthetized as the surgeon destroys the portion of the
nerve that carries the pain.
PSR is effective because it
provides the most lasting pain relief by destroying part of the
trigeminal nerve. PSR provides immediate pain relief for 99% of
patients. Of the 15% of patients whose symptoms recur within 10 years,
medication, repeat PSR, or another surgical procedure will again be
considered. PSR can cause minor complications, such as double vision or
weakness of the jaw. Partial numbness in the area where the pain existed
is a normal side effect. Other complications, such as blurred vision or
chewing problems, are usually temporary (see Percutaneous
Stereotactic Radiofrequency Rhizotomy).
- Percutaneous glycerol rhizolysis is similar to PSR in that a needle is
passed through the cheek to the nerve. However, it uses an injection of
glycerol instead of a heating current to damage some of the trigeminal
nerve fibers that produce pain. This outpatient procedure is performed
under local anesthesia and sedation. The surgeon injects glycerol to
damage the portion of the nerve that carries the pain.
Because
the location of the glycerol cannot be controlled precisely after
injection, the results are somewhat unpredictable. As with PSR, partial
numbness of the face is expected. Other side effects are similar to PSR.
After undergoing percutaneous glycerol rhizotomy, about 70% of
patients have immediate pain relief. In about 50% of patients, symptoms
recur within 3 to 4 years.
- Percutaneous balloon
compression is similar to PSR and
PGR in that a needle is passed through the cheek to the nerve. The
surgeon places a balloon in the trigeminal nerve through a catheter. The
balloon is inflated where fibers produce pain. The balloon compresses
the nerve, injuring the pain-causing fibers. After several minutes the
balloon and catheter are removed.
Complications can be minor
numbness, eye infection, chewing problems, or double vision. The
procedure provides immediate pain relief for 80% of patients. In about
20% of patients who undergo balloon compression, symptoms recur within 3
years.
- Microvascular decompression
(MVD) is the only surgical
procedure that may actually preserve facial sensation, but is the most
invasive. While the patient is under general anesthesia, the surgeon
makes a 1 inch circular opening at the back of the skull called a
craniotomy. This opening exposes the trigeminal nerve at its connection
with the brain. A blood vessel (occasionally a tumor or other
abnormality) is often found that compresses the nerve. After the nerve
is freed from compression, it is protected with a small sponge (see Microvascular
Decompression).
This procedure is effective for 95% of
patients. The major benefit of MVD is that it causes little or no facial
numbness. After MVD, 20% of patients have pain recur within 10 years.
Major disadvantages are the risks of anesthesia and of undergoing an
operation near the brain.
- Neurectomy is the irreversible cutting of the
trigeminal nerve or one of its branches. Cutting the supraorbital nerve,
which supplies sensation to the forehead, may be advised if pain is
isolated to the area above the eyebrow. Cutting the infraorbital nerve
may be performed if pain is limited to the area below the eye along the
upper cheekbone. Cutting
the nerve causes permanent numbness of the region that the nerve
supplies and should only be considered when all other treatments have
failed to control pain. Also, a neurectomy may be performed during an
MVD procedure if no vessel is found compressing the nerve. In this case,
a portion of the trigeminal nerve root is cut at its connection with the
brain.
Questions To Ask Your Doctor
- Is my pain caused by
trigeminal neuralgia?
- Do I need to undergo an
imaging study?
- What treatment is best
for me?
- Can trigeminal
neuralgia be cured?
- How long will I have to
take medications?
- What can I do to help
control my pain?
.


Address: Medlyn Florence
Hospital,St-2 Block "H" North NAZIMABAD Karachi-74700,Pakistan
Phones:
(021)6625584,(021)6678442,(021)6677390 ,Fax :
92-21-6677390,Mobile: 0300-9228559
[email protected]
Web
designed by : Dr.Atiquddin Mallick
Updated : July 13, 2003
Copyright ©Dr.Atiq's Dental
Associates 2001-2002.
![]()