![]()
‘Do I
really need my wisdom teeth extracted?’
There is no routine answer to this question that
applies universally to every person. However, the information below may
help you understand the reasons why people chose to have their wisdom
teeth extracted.
What are impacted wisdom teeth?
Most people have a set of 32 adult teeth. In a
significant number of people, there is not enough ‘room’ in the jaws to
permit the very back molars, or wisdom teeth, to erupt into a proper,
healthy, position (figure 1). This can result in misaligned wisdom teeth
that are able to only partially erupt through the gums, or even not erupt
at all. These teeth are described as ‘impacted’. The wisdom teeth may also
erupt through the gums, but still remain in a poor position because of
their inclination or of the way the gum sits around the tooth. These teeth
are considered to be ‘malpositioned’. Impacted and malpositioned wisdom
teeth both, can lead to gum and tooth disease as well as other worse jaw
disease (see below).

The Decision to Extract ‘Wisdom Teeth’
When making a decision regarding wisdom teeth extraction for patients, surgeons consider the risks and benefits of ‘doing surgery’ against the risks and benefits of ‘not doing surgery’.
Risks of Wisdom Tooth Surgery
In considering wisdom tooth extractions and the risks of doing surgery, you should appreciate that though this risk is relatively small, it is not absolutely zero. There are ‘standard risks’ associated with any type of surgery that include the normal pain, swelling, bruising, bleeding, and infection. There are also other specific risks associated with wisdom tooth surgery and these include being left with a numb lip, chin, or tongue (permanently or temporarily), or a problem with the sinus in the upper jaw. These risks, however, are very uncommon and some even quite rare. Your oral and maxillofacial surgeon will discuss all the risks with you on an individual basis.
Risks of Not Doing Surgery
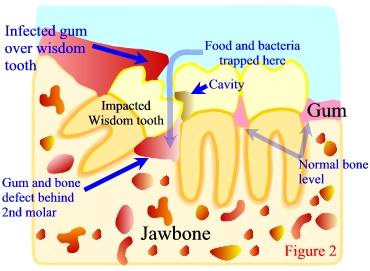
Alternatively, the other question you should ask yourself is ‘What are the risks of not doing surgery and leaving the wisdom teeth behind? When the wisdom teeth erupt through the gums completely, and are able to reach the proper, healthy position in the jawbone, there is little risk in keeping them or ‘not doing surgery’. These properly positioned wisdom teeth are only slightly more likely to develop cavities or gum disease as compared to the other back-teeth in your mouth. However, when a wisdom tooth is impacted or malpositioned, the tooth and associated gum can be very susceptible to bacterial infection, localized gum disease, and gum abscesses. These problems sometimes occur with very little associated pain or discomfort. In such cases, the gum disease and/or infection will progress ‘silently’ until the tooth in front of the wisdom tooth, along with its supporting gum and bone tissue, is damaged. (see figures 2 and 3)
|
X-ray
Picture of Figure2 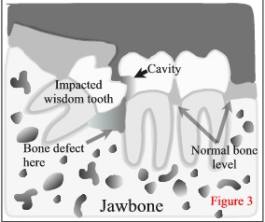 |
Alternativley, impacted or malpositioned wisdom teeth can cause a painful jaw infection with facial swelling, jaw stiffness and pus drainage. Waiting until pain or infection occurs, can result in irreversible damage to adjacent teeth, gum, and the tooth-supporting bone of the jaw. This is why it is often suggested to have wisdom teeth removed early before these events occur. As well, early removal in younger patients can result in more complete healing of any damaged tissues afterwards as compared to removal when patients are older.
Still in other cases, malpositioned or impacted wisdom teeth can cause pain, swelling, jaw stiffness, and pus drainage right from the time they begin to erupt from under the gum and into the mouth. These teeth are also more likely to have cavities in them, which can eventually lead to an ‘abscessed wisdom tooth’.
Click here to see other pictures of impacted teeth and the problems they can cause.
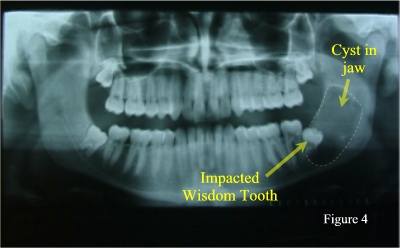
Finally, in rare cases, an impacted wisdom tooth can develop a dental cyst or dental tumour around itself (figure 4).
Impacted Canine Resorbing Lateral Incisor
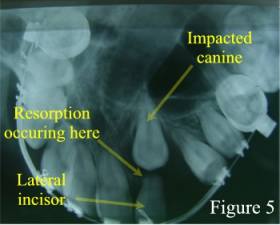
Also, be aware that wisdom teeth aren’t the only teeth that can become impacted. Other teeth in the mouth can also become impacted and cause dental disease (figure 5). These teeth will require extraction as well.
The Final Decision About Your Wisdom Tooth Extractions
At your wisdom tooth consultation appointment, you will be assessed for the need of extraction on an individual basis and an individual treatment plan will be suggested to you. The guidelines below summarize some of the factors that are taken into consideration.
IT IS NOT RECOMMENDED TO HAVE YOUR WISDOM TEETH EXTRACTED IF:
In certain circumstances, oral and maxillofacial surgeons are called upon to extract regular teeth as well. Because an oral and maxillofacial surgeon has a more thorough understanding of medicine, patients who have certain medical concerns are often referred to an oral and maxillofacial surgeon for their dental extractions. Also, you may have been referred because your dentist has determined that an extraction might be particularly risky or difficult. Finally, certain groups of patients who find dental extractions too stressful or anxiety provoking will elect to be referred to an oral and maxillofacial surgeon because they have the ability to administer sedation and general anaesthesia to patients.
The following are some of the most commonly asked questions and concerns regarding “wisdom tooth” extractions and/or common dental extractions.
How much discomfort and pain will I have after the surgery?
Most patients will experience some pain and discomfort after having their wisdom teeth removed. The amount of pain you will have depends upon many factors such as how you react to pain, how difficult your teeth were to remove, how long the freezing lasts, etc. You will likely be given a prescription for painkillers. Take them as directed. The painkillers are not intended to take your pain away completely but you will be more comfortable if you use them as directed.
Will my face swell?
You will most likely experience swelling around your jaws and face after the surgery. Swelling can vary tremendously among patients. Even patients who have had similar extractions can have quite different swelling. The swelling will often be at its worse about two to three days after the surgery. It should gradually subside after this time.
Will I bruise after the surgery?
Every patient is different, but bruising around the jaws is common after wisdom teeth or difficult extractions. The bruising may even track down your neck and even onto your chest. It is important to remember that bruising does not indicate any problems and that it will subside with the passage of time.
How much ‘time-off’ should I plan for?
The amount of school or work you miss and the effects on other daily activities will depend on a number of factors. These include your ability to heal, your pain threshold, your age, whether you have any medical problems, your reaction to anaesthetic drugs, the number and difficulty of your extractions, whether any complications occurred, and post –operative complications like infection or dry socket (see What Is “dry socket”? below ). Generally, plan to miss at least 3-5 days after having 4 impacted wisdom teeth removed (often no time-off is needed for simple extractions). However, more time may be needed for some patients.
What about infection?
Infection after having your wisdom teeth extracted (or even a simple extraction) is not common but can occur. Your doctor will decide whether antibiotics are necessary after your particular extractions. Be aware that infections can still occur even after antibiotics are prescribed. Signs of infection are increased swelling (after the initial “surgical swelling” has begun to decrease), increased pain, persistent bad taste in your mouth, draining pus from the extraction socket or from the gums around the extraction socket, and red, inflamed gums around the extraction socket.
Will I have bleeding after the extraction?
It is common to see blood in your saliva for several hours after the extractions. This is because the extraction sockets may ooze small amounts of blood for the first few hours after the surgery. You may even see tinges of blood on your pillow the next morning. However, significant bleeding after wisdom teeth extractions is very uncommon. DO NOT TAKE ASA (e.g., Bayer) FOR AT LEAST 7 DAYS PRIOR TO YOUR SURGERY DATE AS THIS CAN LEAD TO INCREASED BLEEDING.
What about smoking?
Smoking before and after surgery can cause dry socket (see below) or delayed healing. You should stop smoking completely until the extraction sockets heal, which may take several weeks (If you are unable to completely stop smoking, the less you smoke the better). As well, stop smoking for as long as possible before your surgical appointment.
Will I be completely awake or asleep for my extractions?
This depends on the number of teeth and the difficulty of the extractions. It also depends on how anxious you are about the procedure. Simple extractions can be performed with local anaesthetic (‘freezing’) only. When having all four ‘wisdom teeth’ extracted at once, it is usually more comfortable to receive some form of an oral or intravenous sedative or anaesthetic. Although this will not necessarily put you completely to sleep, patients often think they were put to sleep because they may not remember all or parts of the procedure. For very difficult extractions, you can be put completely to sleep (general anaesthesia) if required. In all cases, you will also be given local anaesthesia or ‘freezing’ in addition to the sedation or anaesthesia so that you will be pain free immediately after the procedure when you wake up, and for several hours afterwards.
What should I eat before the appointment?
If you are receiving intravenous sedation or general anaesthesia in the office, you must not eat or drink anything from midnight before the scheduled procedure. If you do eat or drink anything, you cannot receive any intravenous sedation or general anaesthesia. The only exception to the above is that, if you were prescribed medication to be taken by mouth before the appointment, you may take the prescribed pills with a small amount of water only. If you were prescribed oral sedation only for your surgery, you can eat a light meal up to 4 hours before the procedure.
What about other medication that I may be taking?
First of all, remember to inform the doctor about any medications that you take. This should have been done at your consultation appointment. However, if you think you may have forgotten to mention any drugs or medications at that time, or you are now taking any new medications, inform the doctor before the surgery.
If your take medication for blood pressure, heart conditions, or asthma, continue to take them with a small sip of water the day of surgery. For other medications please remember to check with the doctor.
What is ‘dry socket’?
Dry socket is a fairly uncommon condition that can occur after any dental extraction. You may recognize this condition if the pain returns (after it had already subsided), especially in the area where the tooth was extracted. In addition, pain killers do not seem to work very well. Depending on how much pain you are experiencing, you may have to come into the office to get the socket treated with medication. Dry socket is more common in women, women who take the birth control pill, older people, smokers and in lower jaw dental extractions. Remember that the best treatment is prevention, so if you smoke, stop smoking before and after your extractions.
WISDOM TEETH OR DENTAL EXTRACTIONS
You may experience some difficulty in opening your mouth wide after the surgery, but this will gradually return to normal. Some patients experience difficulty or soreness when swallowing which will also subside. You may feel unwell or run a temperature for a day or so. Also remember that if you had any type of sedation or anaesthesia you may feel tired or run down for one or two days.
Numbness or Altered Feeling/Sensation in Your Lower Lip, Chin and/or Tongue
The roots and jawbone surrounding the lower wisdom teeth can be positioned very close to the nerves that supply sensation to your chin, lip, and tongue. These are the same nerves that your dentist freezes when you get a ‘filling’ in your lower teeth. When removing lower wisdom teeth, these nerves can sometimes be damaged so that even after the local anaesthetic wears off, you would feel the sensation of numbness or an altered sensation in your chin and/or lip and/or tongue. Very rarely permanent numbness or altered sensation of the lip, chin, or tongue can occur. However, permanent numbness is a very rare condition. Usually, high-risk cases can be predicted from the x-rays that are taken before the surgery is done.
Upper Jaw Sinus Involvement
When extracting upper wisdom teeth or upper back teeth, the sinus in your upper jaw can be involved i.e., a hole or opening in the sinus, a tooth fragment remaining in the sinus. This can lead to symptoms like fluids coming out of your nose when you drink or sinus infections. Fortunately, this complication is uncommon. Even if a hole remains after the extraction of a tooth or teeth, more than 95% of cases will heal uneventfully with no lasting complications if you follow instructions properly. Sometimes another surgery will be necessary to close a hole or remove a tooth fragment.
DON’T COMPARE YOURSELF TO YOUR FRIENDS OR ACQUAINTANCES WHO HAVE HAD THEIR WISDOM TEETH EXTRACTED. REMEMBER THAT PATIENTS CAN EXPERIENCE QUITE DIFFERENT CONSEQUENCES AFTER WISDOM TEETH OR EVEN SIMPLE DENTAL EXTRACTIONS.
Some of the conditions which needs immideate attention
Wisdom Tooth Resorbing 2nd Molar
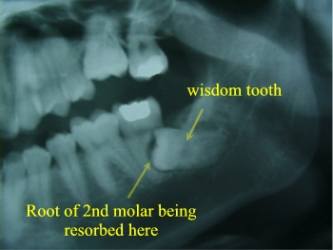
Impacted Wisdom Tooth
Causing Cavity and Bone Loss at the Back of the 2nd Molar
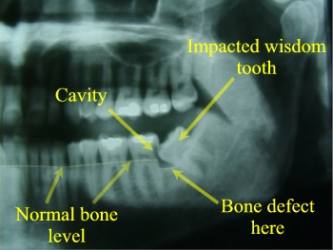
Deep Horizontal
Impaction with Bony Defect Behind 2nd Molar 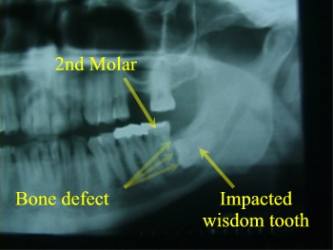
Bony Defect Left After
Wisdom Tooth Extraction in Older Patient 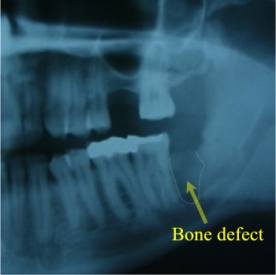
Want to
Know more.........
Web designed by : Dr.Atiquddin Mallick
Updated : July 13, 2003